
Resource Centre
Tools, information and resources to support health professionals and their patients

What are you looking for?
Filter By
13YARN
13YARN: Telephone support and resources

A range of fact sheets and 24-hour telephone crisis support for Aboriginal and Torres Strait Islander peoples experiencing challenges related to mental and emotional wellbeing.
Department of Health and Aged Care
24-hour Movement Guidelines for all Australians – Recommendations

The 24-hour Movement Guidelines outline how much physical activity is recommended each day, limiting sedentary activity, and the inclusion of adequate sleep for children and young people.
National Health and Medical Research Centre
Aboriginal and Torres Strait Islander Guide to Healthy Eating

The Aboriginal and Torres Strait Islander guide to healthy eating is a visual guide of the amount and type of foods recommended for adults for better health and wellbeing. (PDF, 4.3 MB)
Alcohol Drug Information Service
Alcohol and drug clinical advisory service for health professionals

A free telephone support service for health professionals in Queensland, providing clinical advice regarding the management of patients with alcohol and other drug concerns.
Australasian Society of Clinical Immunology and Allergy
Allergy prevention guidelines

Allergy Prevention Guidelines developed by ASCIA to outline practices that may help reduce the risk of infants developing allergies, particularly early onset allergic diseases such as eczema and food allergy.
Tasmanian Government
Appetite for Life: Healthy Ageing

Appetite for life has been developed for use by health and community workers who have direct contact with older people living independently (people over the age of 65). This webpage provides links to download information on practical food ideas, nutrition for managing health conditions, and staying active.
WA Primary Health Alliance
Ask: Starting the conversation about weight

A webpage and video to help health professionals understand weight stigma, and the importance of asking permission to talk about weight with patients. Includes considerations for Aboriginal and Torres Strait Islander patients.
Department of Health Disability and Ageing
Australian 24-hour Movement Guidelines (0-5 years) – Brochure

The 24-hour Movement Guidelines help parents and carers create healthy and safe routines for infants, toddlers and preschoolers. The Guidelines include a picture of what a child’s day during a 24-hour period should look like, including active play, time spent sitting and lying down, and ideal amount of sleep.
Department of Health and Aged Care
Australian 24-hour Movement Guidelines for adults (18 to 64 years) – Recommendations

The 24-hour Movement Guidelines provide information on how much physical activity adults (18 to 64 years) should aim for each day.
Department of Health Disability and Ageing
Australian 24-hour Movement Guidelines for adults and older adults – Report
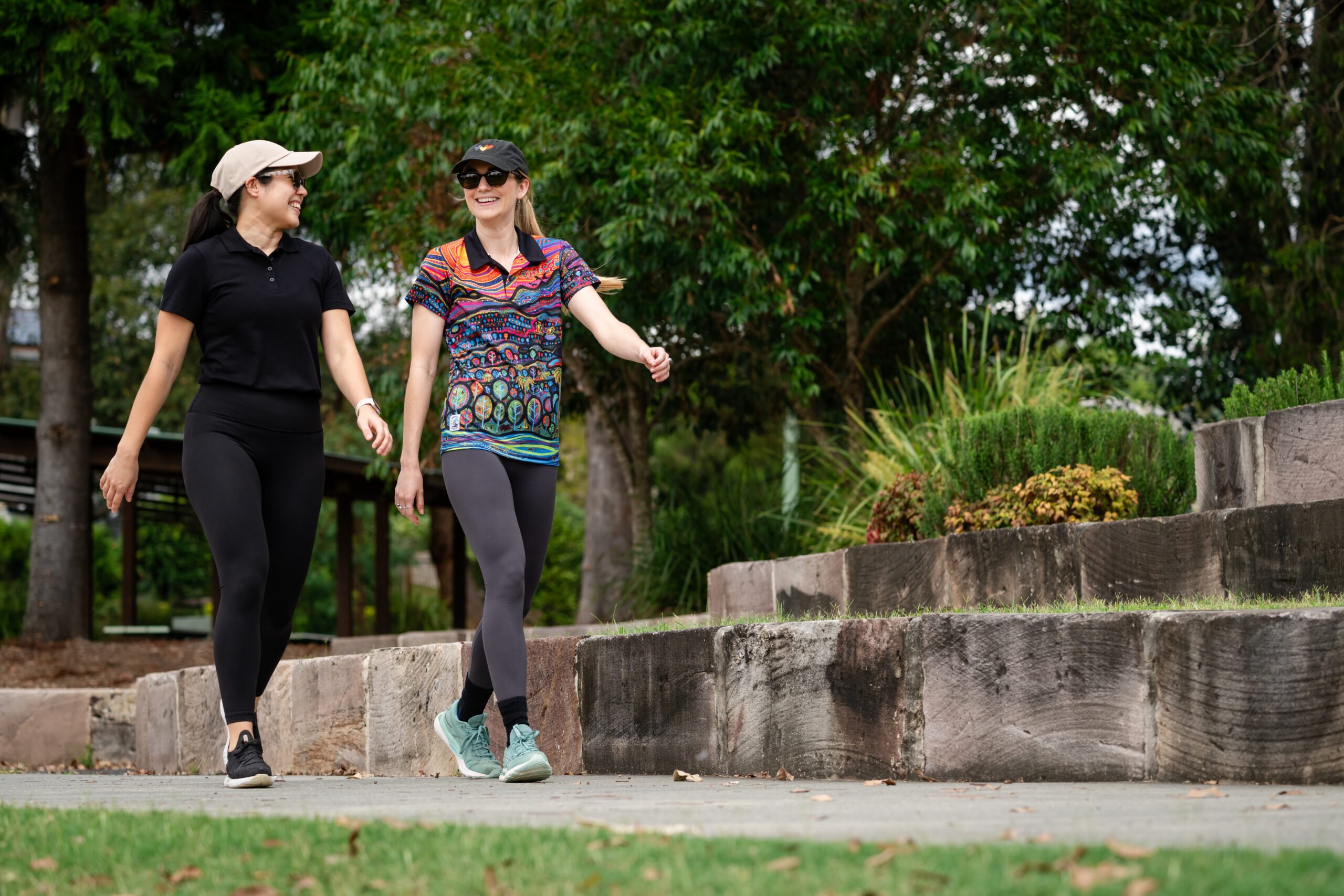
The 24-hour Movement Guidelines outlines a review of the scientific evidence and provides recommendations for adults (aged 18 to 64 years), older adults (65+ years), adults with disability and chronic conditions.
Department of Health Disability and Ageing
Australian 24-hour Movement Guidelines for adults and older adults (18 and over) – Brochure

The 24-hour Movement Guidelines brochure outlines the guidelines for adults, older adults, people with disability and people with chronic conditions, as well as ideas to be active every day.
Department of Health and Aged Care
Australian 24-hour Movement Guidelines for children and young people – Recommendations

The 24-hour Movement Guidelines provide information on how much physical activity children and young people (5 to 17 years) should aim for each day.


